The Healthy Working Lifecycle is at the heart of Sir Charlie Mayfield’s Keep Britain Working report, published in November.
But why should anyone working in workplace wellbeing – especially in smaller organisations and those not chosen ‘vanguards’ for the pilot – pay attention to yet another government commissioned report?
Why not let it gather dust in the bookshelf graveyards where many before them now languish?
Helping work, work
Because this one isn’t about superfluous policy, or the direction of future possible legislation.
It’s about whether work is helping people stay well now. Or making them ill.
And the evidence all points to the latter; the UK has rising economic inactivity due to ill health, longterm sickness absence and a system that too often intervenes late, when problems have already escalated.
Consequently, Simplyhealth’s Angela Sherwood, Chief People Officer, which is a chosen vanguard, describes the government’s focus as “timely and needed”. She adds that the case isn’t just a “moral imperative”, it’s also a “business one” saying that 96% of employers which provide health support see tangible benefits among their workforce.
Creating a resilient workforce
She explains how prioritising Workplace Culture and Employee Health and Wellbeing has impacted Simplyhealth as an employer:
“Embedding wellbeing into our culture has strengthened engagement and resilience, particularly during times of change. Beyond the numbers, it builds trust and loyalty.”
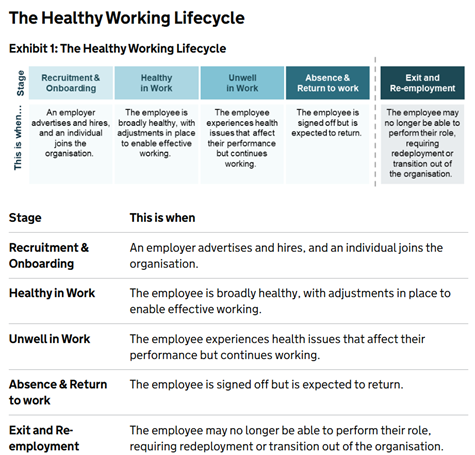
At its simplest, the Healthy Working Lifecycle (HWLC) asks deceptively basic questions:
What are you doing, at every stage of someone’s working life, to keep them healthy, included and able to stay in work? What are you doing to support them to return to work sustainably when things go wrong?
Simple but important
The government describes the lifecycle as “a simple but powerful framework” that reflects “the different stages of a person’s health journey during employment”.
Sherwood defines it as an approach which looks at Employee Health and Wellbeing:
“Holistically across the entire span of an employee’s working life; from onboarding to career progression and through significant life stages such as parenting, menopause and retirement.”
It’s been designed to improve prevention, early intervention, rehabilitation and return to work. But, strip away the labels, and it’s really a challenge to employers to stop treating Employee Health and Wellbeing as something that only matters when someone is already off sick but think about creating better outcomes at each point.
This is not new, and has been talked about in previous government reports, like Working for a Healthier Tomorrow, led by Dame Carol Black.
Why the government is pushing this now
Keep Britain Working report is written in a way that recognises that most employers want to do the right thing. In fact, 87% say they feel responsible for supporting employees’ mental and physical health.
Yet, as the report says, many employers feel trapped in a system that is complex, fragmented and adversarial – with overlapping legislation, inconsistent guidance and a culture that pushes them towards compliance rather than partnership.
3 Main outcomes
So, the lifecycle model is the government’s attempt to flip that dynamic. Instead of focusing on process, it focuses on 3 main outcomes:
- reducing sickness absence
- improving return-to-work rates
- increasing participation and retention of disabled people
Crucially, it is designed to be simple, adaptable and voluntary (at least for now) with the long-term ambition of becoming a shared standard that raises expectations across all workplaces, not just the biggest ones.
It’s understandable that some SMEs don’t feel it’s ‘for’ them compared to large corporations with similarly large budgets for wellbeing.
How do SMEs fit in?
That’s why Jane Austin, HR Director at utilities SME, Wave, is right to stress that the lifecycle:
“Must be relatable, especially to SMEs, which are the bulk of the UK workforce. It’s all very well coming up with recommendations for a big global, but what do they mean for a sub-500 employer?”
As someone responsible for Employ Health and Wellbeing at an SME herself, she knows implementing the lifecycle doesn’t have to be costly (more on actions that can be taken in a follow up feature next) and looks forward to hearing recommendations that work for all.
Mixed reactions
There’s inevitably mixed reactions to the report, both interest and scepticism. Especially as employers are already under a lot of pressure ,with everything from NIC hikes to a cost of living crisis. Budgets are tight. And Employee Health and Wellbeing initiatives that don’t show immediate return can feel like a luxury.
But several professionals we spoke to argue that this is precisely where the lifecycle approach earns its keep.
As Dr Samantha Philips, Head of Health and Wellbeing at TfL, Transport for London, points out, keeping people well and in work is almost always cheaper than losing them: recruitment costs, training time, lost productivity, and the risk of having to start again if a hire doesn’t work out.
“If you do things that keep your employees at work or help them come back to work,” she says “ultimately that has to save you money.”
Moving from “fixing” health to creating good work
Luke Bullen, Head of UK & Ireland, wellhub, describes the Healthy Working Lifecycle as a move away from the idea that poor health is either an individual’s responsibility, or something the NHS steps in to fix.
Instead, it positions good work itself as a driver of good health.
A lifecycle approach acknowledges that people move in and out of challenges across their working lives and that how employers respond makes a significant difference to outcomes.
His inhouse data backs this up. Wellhub’s Return on Wellbeing research shows that organisations taking a lifecycle approach see stronger retention, lower absenteeism and measurable productivity gains. In a labour market where 93% of employees now rate wellbeing as highly as salary, this is increasingly about competitiveness as much as care.
Not “another corporate word”
Of course, language matters, and not everyone loves the term itself.
“You don’t need to mention the lifecycle at all, we don’t,” says Austin.
“Just have it in mind. If you asked our people what keeps them here, it’s culture and wellbeing. If you feel well treated across your career, and particularly at those times you have personal problems or your health dips, then not only will you give back to that employer, you are far more likely to be able to stay in work, knowing you’re supported and that you matter.”
She adds that employers shouldn’t see times when employees are too ill to be in work as “a failure” but as an “opportunity to stay in touch”, support them and know they will be welcomed back in a “sensitive” way.
Applying the thinking of the report
That sentiment comes up repeatedly. For many employers, especially smaller ones, success won’t come from adopting the terminology but from applying the thinking.
Sally Pritchett, Chief Executive of another SME, communications company Something Big, agrees. For SMEs without dedicated wellbeing specialists, the lifecycle can act as a useful lens; a reminder that Employee Health and Wellbeing needs attention at every stage of work to keep them well.
And, she argues, the most effective actions often cost nothing at all: honest conversations, flexibility, trust, and small human adjustments that prevent disengagement, absence and churn later on.
Why this matters beyond individual businesses
There is also a wider argument running through the report that businesses do not operate in isolation.
As Philips highlights, when the NHS is under strain and mental health challenges are rising, the cost shows up somewhere. Employers feel it through absence, burnout and turnover. The UK as a whole feels it through lost participation and productivity.
This is why the Healthy Working Lifecycle is framed as a collective movement.
As one HR Director at a consultancy puts it, the obsession with high performance often misses the point: if people are not well, performance suffers anyway. Burnout, anxiety and sickness come at a cost that is human and commercial.
A framework, not a silver bullet
There are legitimate questions about implementation. One HR professional raises concerns about whether the right stakeholders are being engaged, and whether the buck will stop with HR, line management, or C-suite – and whether the people driving change will be well supported enough themselves.
But most contributors agree on one thing: the Healthy Working Lifecycle does not claim to be a silver bullet.
It is a useful framework. And the best thing about it? It does not require employers to wait for legislation, accreditation or incentives. It asks them to look honestly at what they are already doing and where people are falling through the cracks now.
Many agree that we’ve reached a tipping point when it comes to keeping people well, which is ultimately the only thing that will keep business, and the country, working at all.
You might also like:













